Exceptional Services We Offer
We are a private practice specializing in the area of Cardiac Electrophysiology. We are dedicated to the treatment of patients with heart rhythm disturbances. Our patients have a broad range of arrhythmias ranging from palpitations to sudden cardiac arrest. We have access to some of the most advanced treatments available for diagnosing and treating heart rhythm problems. More importantly, we have the experience and knowledge necessary to approach these difficult problems.
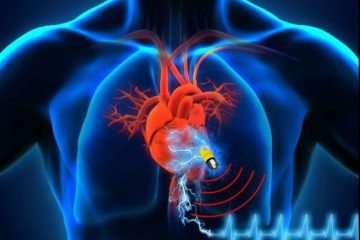
Pacemakers
PacemakersPacemakers A pacemaker is a treatment for an abnormally slow heart beat that if left untreated, can lead to weakness, confusion, dizziness, fainting, shortness of breath and...
READ MORE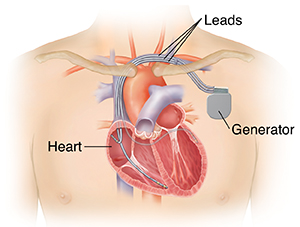
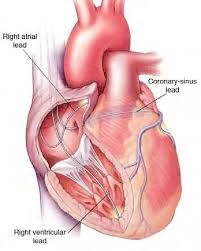
Biventricular Pacemaker/ICDs
Biventricular Pacemaker/ICDsBiventricular Pacemaker/ICDs Biventricular Pacemaker/ICDs are specially designed devices used to address a condition in which the left and right sides of...
READ MOREAbout Our Company
The mission of Cardiology & Arrhythmia Consultants P.C. is to always deliver the highest quality of cardiovascular care for its southeastern Michigan patients, to always serve as an advocate for patient needs and to provide unyielding support to the primary care physicians.
The vision of Cardiology & Arrhythmia Consultants P.C. is to cultivate an environment of care that relieves patients of suffering in the most humane way possible, and to expedite their restoration of function through a pleasant experience during all aspects of treatment. Dr. Goel provides patients with optimal value and uncompromised service at a fair price. And renders cardiovascular care to all who request our services regardless of their social, economic status, race, or religious preference. Dr. Goel strives to attain clinical and psychological excellence for the total healing of our patients.
Schedule Appointment
Why Choose Us?
Accepted Insurance
We accept most of the Health Insurance.Dependable Services
We love to take pride in the work we do. Each project is finished in time and budgetNext Previous Client Testimonials
I was always having congestive heart failure, shortness of breath and did very little activity for fear of having a bad day. If I went down steps to do laundry, I couldn't come back up the steps. Dr. Anil Goel suggested an InSync Maximo defibrillator implant for better qualityu of life. On February 10, 2005, I had the implant done. Today, three years later at the age of 78, I am able to go on short walks, go up and down the steps to do my own laundry, stand on my feet to cook and wake up every day knowing it's going to be a better day.
I am 74 years old. I have had several heart problems over decades. I had my first heart surgery 24 years ago and another in 2000. I have 11 stents in my heart. Three years ago I was referred to Dr. Goel due to fainting spells. He recommended a pacemaker defibrillator to prevent dangerous heart rhythms that were leading to fainting. He performed the procedure in 2004 and everything went just fine. I Know Dr. Goel was the right person to do my surgery. A lot my friends have had this done elsewhere and they have had many problems.
"I have had a heart condition with congestive heart failure for 13 years. Thirteen years ago I had a six-way bypass and a heart device implanted since then. Two years ago I could hardly get out of bed due to weakness, shortness of breath and swelling. I was told there is no hope of improvement in my circumstances. I was referred to Dr. Goel by my cardiologist Dr. Thomas Mathew for consideration of biventricular pacemaker and Dr. Goel suggested upgrading my device to a biventricular defibrillator.
Almost three years ago I experienced Atrial Fibrillation that put me into Beaumont Hospital for almost a week. At that time I was assigned the doctor on duty and ended up with a pacemaker and a list of drugs. The treatment and the drug regime did nothing to prevent Atrial Fibrillation or improve my general health. During the next year and many tests and procedures, my Atrial Fibrillation continued and got worse, as did my health and attitude.
I have been a patient of Dr. Anil Goel for 16 years. He is an extremely competent physician and has always been empathetic and helpful. His staff is caring and efficient. Of course there is clinical professionalism, but it is also blended with a friendly and calming atmosphere.