 An Implantable Cardioverter Defibrillator, or ICD, connects to leads positioned inside the heart. These leads are used to deliver controlled electrical shocks to reset the heart should its rhythm become so abnormal as to be life threatening.
An Implantable Cardioverter Defibrillator, or ICD, connects to leads positioned inside the heart. These leads are used to deliver controlled electrical shocks to reset the heart should its rhythm become so abnormal as to be life threatening.
Biventricular Pacemaker/ICDs
Biventricular Pacemaker/ICDs are specially designed devices used to address a condition in which the left and right sides of a person’s heart are no longer synchronized. The ICD, or implantable cardioverter defibrillator function, acts as a reset device for the heart, jolting it with an electrical shock to restore the heart beat to normal in certain critical circumstances (to learn more about implantable cardioverter defibrillator, click here).
A Biventricular Pacemaker/ICDs is designed to treat the delay in heart ventricle contractions by causing the two sides to once again beat in sync, relieving the symptoms of heart failure and improving the person’s overall quality of life.
The heart
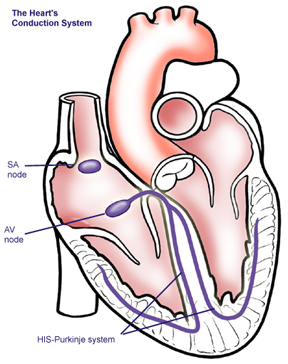 The heart is made up of four main cavities–the right and left atriums are the top two chambers of the heart and the right and left ventricles are the bottom chambers of the heart.
The heart is made up of four main cavities–the right and left atriums are the top two chambers of the heart and the right and left ventricles are the bottom chambers of the heart.
In a normal heart, the left and right sides of the heart beat together to maintain a steady supply of blood and oxygen to the rest of the body.
A typical heart beat begins with the sinoatrial node, a cluster of specialized cells located in your right atrium, firing an electrical impulse that spreads through the walls of the right and left chambers, causing them to contract, thus forcing blood into the lower chambers.
The impulse then travels to the atrioventricular node, another center of special cells located in the lower part of the right atrium. After a short pause, the pulses travels into the lower chambers, causing them to contract, forcing blood out of the heart to the lungs and body.
In a weakened heart, blood moves through the heart and body at a slower rate than normal and pressure in the heart increases, which over time can cause problems. Specifically, it can result in a delay between the contraction of the two sides. When this happens, the walls of the left ventricle are unable to contract at the same time as the right ventricle, leading to an increase in heart failure symptoms, such as shortness of breath, dry cough, swelling in the ankles or legs, weight gain, fatigue, or rapid or irregular heart beat.
How does a Biventricular Pacemaker/ICDs work?
A pacemaker is a device that sends electrical impulses to the heart muscle to maintain a suitable heart rate and rhythm. The pacemaker has two parts: the pulse generator and leads (think very fine wires). The pulse generator houses the battery and a tiny computer. The computer tracks the heart’s electrical activity and also stimulates the heart by sending impulses directly to the heart along the leads.
Traditional pacemakers are used to treat slow heart rhythms. Such pacemakers use one or two leads to sense and pace the right lower chamber, and sometimes the right upper chamber.
With a Biventricular Pacemaker/ICDs, leads are implanted through a vein into the upper right chamber and lower right chamber, like a traditional pacemaker, with a third lead being implanted in the lower left chamber.
In this way, the device can directly stimulate three chambers of the heart, helping it beat in a more balanced way. You may have heard this process called “cardiac resynchronization therapy.”
Biventricular pacing keeps the right and left lower chambers pumping together by sending small electrical impulses through the leads. This allows the left and the right chambers to pump together with the end result being the heart is able to fill and pump blood more efficiently.
Who is a candidate for a Biventricular Pacemaker/ICDs?
Biventricular Pacemaker/ICDs/ICDs improve the symptoms of heart failure in about 70 percent of patients that have been treated with medications but still have severe or moderately severe heart failure symptoms.
To be eligible for the Biventricular Pacemaker/ICDs, heart failure patients:
- have severe or moderately severe heart failure symptoms;
- are taking medications to treat heart failure; and,
- have delayed electrical activation of the heart.
In addition, the heart failure patient may or may not need this type of pacemaker to treat slow heart rhythms and may need an internal cardioverter defibrillator (ICD), which is designed to treat patients at risk for sudden cardiac death or cardiac arrests.
What can I expect as a Biventricular Pacemaker/ICDs recipient?
After you are diagnosed as a candidate for biventricular pacemaker/ICD insertion, you may be asked to stop taking certain medications several days before your procedure (such as blood thinners and aspirin). If you are a diabetic, you may be asked to adjust your diabetic medications. Do not eat or drink anything after midnight the night before the procedure. If you must take medications, drink only small sips of water to help you swallow your pills.
When you get to the hospital you will change into a hospital gown for the procedure, which will be performed in the Electrophysiology Lab. You will lie on a bed and the nurse will start an intravenous line to deliver medications and fluids.
You will receive a medication through your IV to make you very drowsy. The medication will put you to sleep. Due to the medications you will likely not recall the procedure afterwards.
This is completely normal.
Prior to the procedure, the nurse will connect you to several monitors that will allow the medical staff to monitor your condition at all times during the procedure.
The staff will clean and shave the area of the incision and you will be covered with a sterile cloth, after which the doctor will numb your skin by injecting a local anesthetic in the shoulder area. You may feel a slight pinching or burning feeling at first and then the area will become numb.
After you are numb, an incision will be made to insert the pacemaker and leads.
During the procedure, two very fine wires will be placed into a vein and the doctor will use a fluoroscopy machine (a special x-ray machine that allows the doctor to see your blood vessels), to guide them into the upper and lower right chambers of your heart. The lead tips are attached to your heart muscle. A third very fine wire is guided through your vein to a small vein on the back of the heart called the coronary sinus to pace the left lower left chamber. The other ends of the leads are attached to the pulse generator, which is placed under the skin in the upper chest, just below your shoulder.
After the leads are in place, the physician tests the leads to make sure lead placement is correct, the leads are sensing and pacing appropriately and the right and left ventricle are synchronized. This is called “pacing” and involves delivering small amounts of energy through the leads into the heart muscle. This causes the heart to contract.
After the leads are tested, the doctor will connect them to your Biventricular Pacemaker/ICDs/ICD. The rate of your pacemaker and other settings will be determined by your doctor. The final pacemaker settings are done after the implant using a special device called a “programmer,” which is used to put your heart into a fast rhythm so the doctor can watch as the device does its job–this all occurs as you are still sound asleep.
The biventricular pacemaker implant procedure may last about two to five hours as in an enlarged heart due to heart failure, the third lead placement can be difficult to place and find the perfect “spot” to synchronize the chambers.
After the pacemaker implant?
After the pacemaker implant, you will be admitted to the hospital overnight where your heart will be monitored for rate and rhythm. The following morning, you will sometimes have an x-ray to check your lungs and the position of your pacemaker.
Before being released from the hospital, your device will be tested one last time. The nurse or technician will place tiny electrodes onto your chest that attach to a computer monitor by a cable. A small machine known as a programmer is used to check your biventricular pacemaker/ICD. It has a wand that is placed directly over the device. This programmer allows the nurse or technician to read your pacemaker settings and check the wires(leads).
With the programmer, the function of the pacemaker and leads can be evaluated. You may feel odd or feel your heart beating faster.
This is normal; however, report all symptoms to the nurse. Results of the pacemaker check are discussed with your doctor who will then determine your pacemaker settings.
Going home
Usually, you will be able to go home the day after your pacemaker was implanted. Your doctor will discuss the results of the procedure and answer any questions you may have.
Keep the area where the pacemaker was inserted clean and dry. The next day you may take a shower. Look at the area of the surgery daily to make sure it is healing. Your incision will be bound by surgical tape on the surface–leave these in place (the doctor will remove them at your follow up visit, though if they fall off on their own this is OK). Call your doctor if you notice unusual redness, swelling, drainage from your wound, or if you experience fever or chills. A biventricular device is bigger than other pacemakers, so you will probably always see and feel it.
You will be restricted in movement for the month following the procedure. You should not lift your elbow above your shoulder. You should not life heavy objects. Activities such as golf, tennis and swimming should be avoided for six weeks after the pacemaker was implanted.
Despite what you may have heard, microwave ovens, electric blankets and heating pads may be used. Cellular phones can be used on the side opposite your device. You should receive a booklet with a lot of information about your device after surgery. If you do not, ask.
Directly after the procedure, you will receiver a temporary pacemaker ID card that tells you what type of pacemaker and leads you have, the date of implant and the doctor who implanted it. In about two months, you will receive a permanent card from the company. It is important that you CARRY THIS CARD AT ALL TIMES in case you need medical attention at another hospital.
If you will be traveling through an airport, present this card to the security personnel (go to the front of the line) and they will scan you with a portable wand, rather than require you to step through the walk-through detectors. (your device will set off the alarm). The wand will not damage the pacemaker.
Ask your doctor or nurse for more specific information regarding what types of equipment may interfere with your pacemaker.
Follow-up care
About two weeks after the procedure, you should see your doctor for a complete pacemaker check. This check is very important as adjustments will be made that can prolong the life of the pacemaker. You should also visit your doctor every three to four months following implantation to ensure everything is operating properly.
If I get a shock…
In addition to pacing and synchronizing the beating of your heart, your device may has a third function–it acts as an implantable cardioverter defibrillator to shock the heart should it start beating too fast. The shock resets the heart to its normal pumping rate.
If you get one shock, and feel OK, call the office and make an appointment for the next available opening. Be sure to tell the assistant that you received a shock from your device.(It’s O.K.–it’s doing its job)
If you receiver two shocks in a short period of time, or two shocks in a day, go to the nearest hospital. There may be something going on with your heart and you need to be monitored.
How long will my pacemaker last?
Biventricular devices usually last anywhere from 4 to 6 years, so it is important that you maintain a regular schedule of visits with your physician so he or she can monitor its status. How long your device will last depends on how hard the battery inside the device has to work. This is affected by how much energy is required to pace the heart and how the system is programmed. Thanks to ongoing research and development, the life of pacemakers and ICD’s continues to increase as their size decreases, making them more comfortable for people.

